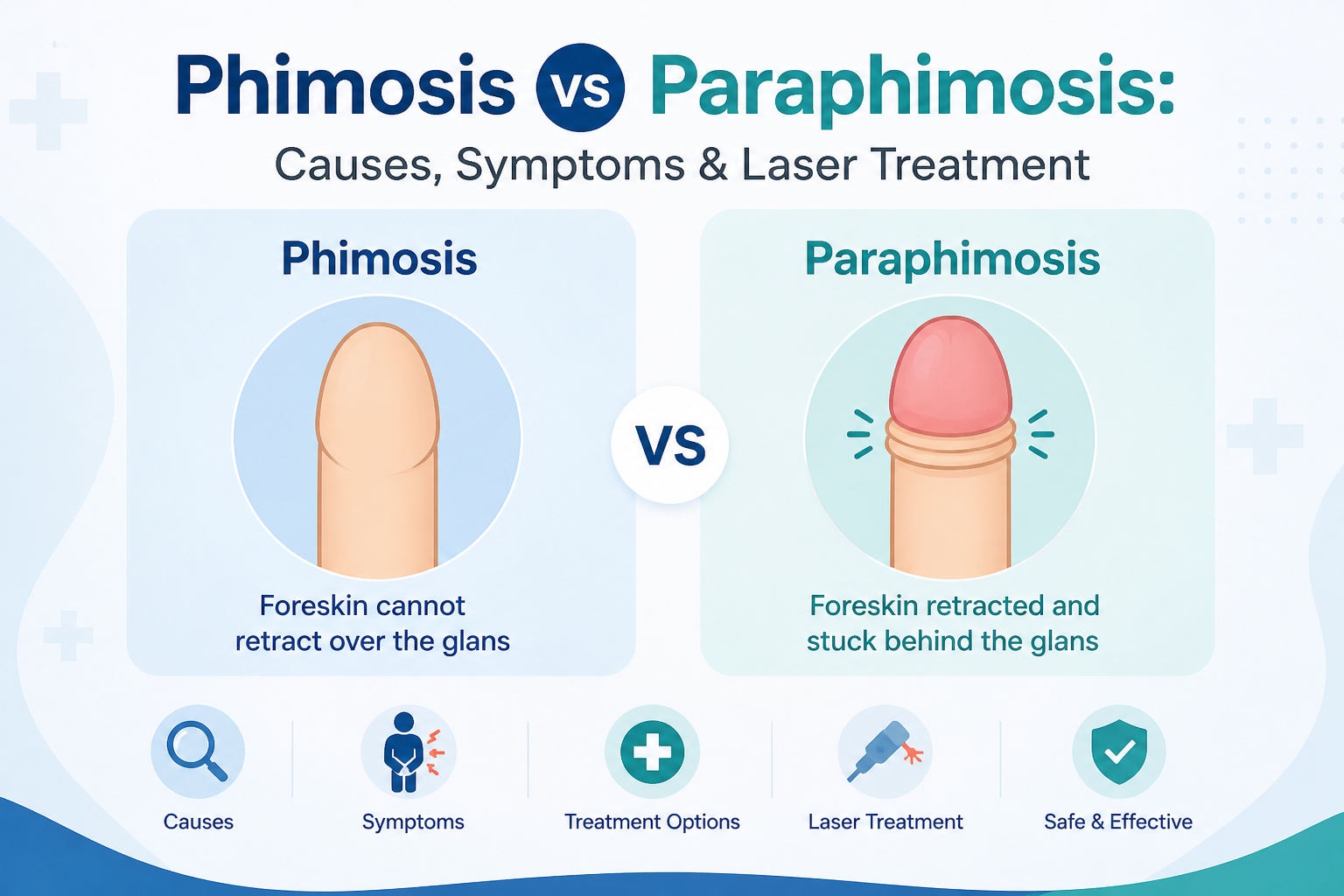

Foreskin conditions are among the most misunderstood areas of male health. Men frequently delay seeking help due to embarrassment, and parents often worry unnecessarily when their young children show normal developmental tightness. Understanding what phimosis and paraphimosis actually are - and how different they are from each other - is the foundation for making the right decision about treatment.
Understanding Foreskin Conditions in Men
In uncircumcised males, the foreskin (prepuce) is a fold of skin that covers the head (glans) of the penis. It is designed to retract freely, exposing the glans during sexual activity and for hygiene purposes. When this retraction is impaired - either because the foreskin is too tight to pull back, or because it has been pulled back and cannot return - a medical condition exists.
These two scenarios define phimosis and paraphimosis respectively.
What is Phimosis?
Phimosis is the inability to retract the foreskin over the head of the penis. The foreskin is too tight to be pulled back freely, either partially or completely.
Phimosis exists in two clinically distinct forms:
Physiologic Phimosis
This is the natural, normal state of the foreskin in infants and young boys. At birth, the inner surface of the foreskin is attached to the glans by natural tissue adhesions. Over time - typically by age 3 and almost universally by the mid-teens - these adhesions separate and the foreskin becomes retractable on its own.
- In boys under 4 years old, inability to retract the foreskin is completely normal
- By age 10–11, most boys can partially or fully retract the foreskin
- By age 17, the vast majority of males have full foreskin retraction
Physiologic phimosis requires no treatment. Forcing retraction before it occurs naturally is harmful and can cause scarring, injury, and paradoxically worsen the condition.
Pathologic Phimosis
Pathologic phimosis is a disease process - it occurs when the foreskin becomes tight or scarred due to an underlying cause. It can affect boys who previously had normal foreskin function and is more common in adults.
Common causes of pathologic phimosis include:
- Balanitis - recurring inflammation or infection under the foreskin
- Lichen sclerosus (balanitis xerotica obliterans) - a chronic skin condition that causes white, hardened patches and scar tissue on the foreskin and glans, making it progressively inelastic
- Forceful retraction - tearing the foreskin prematurely creates scar tissue that tightens the skin
- Diabetes - increases susceptibility to fungal and bacterial infections under the foreskin
- Eczema and psoriasis - skin conditions that can affect the penile skin and foreskin
- Poor penile hygiene - chronic irritation from smegma accumulation leads to infection and fibrosis
What is Paraphimosis?
Paraphimosis is a urological emergency. It occurs when a tight foreskin is pulled back behind the head of the penis and then becomes trapped - unable to return to its normal forward position.
Once the foreskin is stuck behind the glans, it acts as a tourniquet. The constriction ring formed by the tight foreskin compresses the veins and lymphatic vessels, causing the glans to swell rapidly. As the glans swells, it becomes progressively harder to slide the foreskin back forward - creating a self-worsening cycle.
If blood flow to the glans is fully restricted, the tissue begins to suffer from oxygen deprivation. In severe cases, this can result in tissue death (gangrene) of the penile tip - a catastrophic and permanent injury. A dark purple or black discolouration of the glans is a sign that blood supply has been critically compromised and immediate emergency intervention is required.
Phimosis vs Paraphimosis - Key Differences at a Glance
Causes of Phimosis
In children, physiologic phimosis is simply developmental. In older boys and men, pathologic phimosis results from:
- Recurrent foreskin infections (balanitis or balanoposthitis)
- Scar tissue from forced retraction or injury
- Lichen sclerosus - the most common cause of pathologic phimosis in adults
- Inflammatory skin conditions (eczema, psoriasis, dermatitis)
- Diabetes - increases risk of recurrent fungal and bacterial infections
- Sexually transmitted infections causing inflammation and scarring
Causes of Paraphimosis
Paraphimosis always begins with a foreskin that has been retracted and not returned to its natural position. Common triggers include:
- Medical procedures - catheters, cystoscopies, or penile examinations where the foreskin is pulled back and not replaced afterward (a preventable medical error)
- Sexual activity - retraction during intercourse or masturbation without replacing the foreskin
- Pre-existing tight foreskin - men with mild phimosis who force retraction are at higher risk
- Penile piercing - jewellery can prevent the foreskin from returning forward
- Prolonged retraction - simply forgetting to replace the foreskin after cleaning
This is why medical teams are trained to always push the foreskin forward after any penile procedure or catheter insertion.
Symptoms of Phimosis
In physiologic phimosis (children), there are typically no concerning symptoms - the foreskin simply does not retract, which is normal.
In pathologic phimosis in older boys and adults, symptoms include:
- Inability to pull back the foreskin - partial or complete, beyond the age when full retraction is expected
- Pain during erection or sexual intercourse - the tight foreskin cannot accommodate the expanded glans
- Ballooning of the foreskin during urination - urine collects under the foreskin before passing through, indicating a narrowed opening
- Recurrent infections under the foreskin - redness, swelling, discharge, or odour from the glans area
- White ring of tightened skin - a visible constricting band at the tip of the foreskin, particularly associated with lichen sclerosus
- Difficulty with penile hygiene - inability to clean under the foreskin, leading to smegma build-up and increased infection risk
Symptoms of Paraphimosis
Paraphimosis presents dramatically and worsens quickly. Recognise these warning signs and treat them as urgent:
- Foreskin retracted and stuck - the foreskin cannot be pulled forward over the glans
- Rapid, painful swelling of the glans - the head of the penis becomes enlarged and tender
- A visible constricting ring behind the glans - the trapped foreskin creates a painful band
- Severe pain in the penis - worsening over time as swelling increases
- Skin colour changes - the glans may turn bright red, then dark purple or blue as blood flow is increasingly restricted
- Numbness or coldness - late signs indicating significant vascular compromise
Any case of paraphimosis requires immediate medical attention. Do not attempt to force the foreskin forward at home if significant swelling is already present - this can worsen the injury.
Diagnosing Phimosis and Paraphimosis
Both conditions are diagnosed through clinical examination. No imaging is typically required.
For phimosis, a doctor assesses:
- The degree of retraction possible
- The presence of scarring, white plaques (lichen sclerosus), or inflammation
- Whether symptoms affect urination or sexual function
- Underlying conditions such as diabetes or recurrent balanitis
For paraphimosis, diagnosis is immediate and visual - the trapped, swollen configuration is unmistakable. The priority is assessing blood flow to the glans and initiating reduction immediately.
Treatment Options for Phimosis
Treatment depends on the severity of symptoms and whether the condition is physiologic or pathologic.
Steroid Creams
For mild to moderate phimosis in older boys and adults, topical corticosteroid cream (such as betamethasone or hydrocortisone) is the recommended first-line treatment. Applied to the tight area of the foreskin two to three times daily for four to eight weeks, steroid creams reduce inflammation and improve skin elasticity - allowing gradual retraction without surgery.
Success rates range from 70–90% in appropriate cases. This approach is particularly effective when combined with gentle stretching exercises and good hygiene.
Foreskin Stretching Exercises
Gentle manual stretching of the foreskin - performed regularly over several weeks - gradually widens the tight opening. Done carefully and without causing pain or tearing, stretching can resolve mild phimosis without any medical intervention. It is most effective when used alongside steroid cream for pathologic cases.
Preputioplasty (Foreskin-Preserving Surgery)
For men who want to retain their foreskin but need surgical correction, preputioplasty is a foreskin-widening procedure. A small incision is made at the tight ring of the foreskin to release the constriction, then the skin is sutured in a way that widens the opening without removing the foreskin. Recovery is faster than circumcision and the foreskin is preserved.
Laser Circumcision
Laser circumcision is an advanced, minimally invasive technique that uses a precisely controlled laser beam to remove the foreskin instead of a scalpel. It is increasingly the preferred approach in contemporary urology for the following reasons:
How it works: A CO2 or diode laser is used to cut and simultaneously seal blood vessels as the foreskin is removed. This precision eliminates the main disadvantages of traditional surgery.
Advantages of laser circumcision over traditional surgery:
- Minimal bleeding - the laser cauterises blood vessels as it cuts, dramatically reducing intraoperative blood loss
- Lower infection risk - the sealed wound is cleaner and less prone to post-operative infection
- Reduced pain - the laser causes less tissue trauma than a scalpel, resulting in a more comfortable recovery
- Faster recovery time - most men return to normal activity within 5–7 days, compared to 2–3 weeks for traditional circumcision
- Greater precision - the laser allows the surgeon to control the depth and area of removal exactly, producing a neater cosmetic result
- Suitable for all grades of phimosis - including cases involving lichen sclerosus and significant scarring
Laser circumcision is performed under local or general anaesthesia as a day procedure. It is particularly beneficial for adult men with pathologic phimosis who have not responded to steroid cream or stretching.
Traditional Circumcision
Standard surgical circumcision - removal of the foreskin using a scalpel - remains effective and is widely performed for phimosis. It is the most common definitive treatment for pathologic phimosis in adults. Recovery typically involves 2–3 weeks of healing. Traditional circumcision is appropriate when laser technology is not available or when the clinical situation warrants it.
Treatment for Paraphimosis - A Medical Emergency
Paraphimosis must be treated immediately. The goal is to reduce the swollen glans and slide the foreskin forward over it. Treatment options depend on the degree of swelling and vascular compromise.
Initial manual reduction (mild cases):
- Ice packs or cold compression applied to the glans to reduce swelling
- Firm, steady manual compression of the glans to reduce its size
- Once adequately compressed, the foreskin is pushed forward over the glans with controlled pressure
- Lubricating jelly may assist the process
Medical intervention (moderate to severe cases):
- Injection of hyaluronidase enzyme into the swollen tissue to reduce oedema and allow manual reduction
- Needle puncture of the oedematous tissue to release fluid and decompress the glans
Emergency surgical intervention (severe cases):
- A dorsal slit procedure - a vertical incision through the constricting band - immediately releases the compression
- Emergency circumcision may be performed to resolve the paraphimosis and prevent recurrence permanently
Following successful reduction, circumcision is typically recommended to prevent paraphimosis from recurring.
Why Laser Circumcision is Gaining Preference
Men seeking treatment for phimosis are increasingly choosing laser circumcision over traditional surgery for one central reason: recovery quality. The combination of less pain, reduced bleeding, lower infection risk, and faster return to normal life makes laser the superior patient experience in the vast majority of eligible cases.
From a clinical perspective, laser precision also reduces the risk of taking too much or too little foreskin - a cosmetic and functional concern in traditional circumcision. The sealed wound requires less post-operative care and dressing changes.
For adult men in whom steroid cream and stretching have failed, laser circumcision represents the most comfortable and efficient path to a permanent resolution of phimosis.
Expert Tips for Foreskin Health
These practical insights support better outcomes - whether managing phimosis conservatively or preparing for treatment:
- Never force foreskin retraction in a child. The single most common cause of pathologic phimosis in boys is premature forced retraction by well-meaning parents or caregivers. The foreskin separates naturally - let it happen on its own timetable.
- Hygiene under the foreskin matters, but not aggressively. Gentle rinsing with warm water is sufficient. Soap and antiseptics under the foreskin disrupt the natural flora and can cause the irritation they are meant to prevent.
- Steroid cream works - but only with the right technique. Apply to the tightest part of the foreskin and gently stretch the skin as you apply. Using it on the outer shaft rather than the constricting ring produces no benefit.
- If the foreskin won't come forward - go to A&E immediately. Every hour of delay in paraphimosis allows more swelling to accumulate and makes manual reduction harder. Time is the most critical variable.
- Recurrent balanitis is a warning signal. If you or your child is experiencing frequent penile infections, see a GP. Chronic balanitis is both a cause and a complication of phimosis, and breaking the cycle early prevents the need for surgery in many cases.
Conclusion
Phimosis and paraphimosis are two distinct foreskin conditions that are frequently confused - but clinically, they could not be more different in urgency or approach. Phimosis is common, manageable, and treatable at every severity level from cream to laser. Paraphimosis is an emergency that demands immediate attention to prevent permanent injury.
Key takeaways:
- Phimosis in children is usually normal and resolves without any treatment
- Pathologic phimosis in adults is caused by scarring, infection, and skin conditions - and it is treatable
- Paraphimosis occurs when a retracted foreskin becomes trapped - it is always a medical emergency
- Steroid cream and gentle stretching are effective first-line treatments for mild phimosis
- Laser circumcision offers a minimally invasive, faster-recovery alternative to traditional surgery for those who need definitive treatment
- Paraphimosis that has caused significant swelling or colour changes requires emergency medical care - do not delay
If you are experiencing symptoms of either condition, the right time to seek medical advice is now - not after it worsens.