
You notice discharge in your underwear - again. It's white, maybe slightly thick, and you're not sure if it's just your body doing its thing or a sign that something is wrong. You search online and land in a spiral of alarming possibilities.
Here's the truth: white vaginal discharge is one of the most common - and most misunderstood - aspects of women's reproductive health. Most of the time it's completely normal. But sometimes it's your body's way of flagging an infection that needs attention.
In this guide, you'll learn exactly what leucorrhea is, how to read the signals your discharge is sending, and practical do it yourself steps to assess, manage, and prevent abnormal discharge - so you know with confidence when to act and when to relax.
What is Leucorrhea and Why Does It Happen?
Leucorrhea is the medical term for white or whitish vaginal discharge. It is a natural, ongoing process that every woman experiences throughout her reproductive life. Far from being something to be ashamed of or worried about, it actually plays a protective role for your body.
Vaginal discharge is produced by the cells and glands inside the vagina and cervix. Its primary jobs are to:
- Flush out dead cells and bacteria from the vaginal canal
- Maintain a healthy pH balance inside the vagina
- Protect the reproductive tract from infection
- Signal hormonal changes, including ovulation and pregnancy
Is White Discharge the Same as Leucorrhea?
Yes - leucorrhea specifically refers to white or off-white vaginal discharge. It is not a disease on its own. It is a symptom or sign that can be either physiological (normal) or pathological (caused by infection or illness). The key is understanding which type you're dealing with.
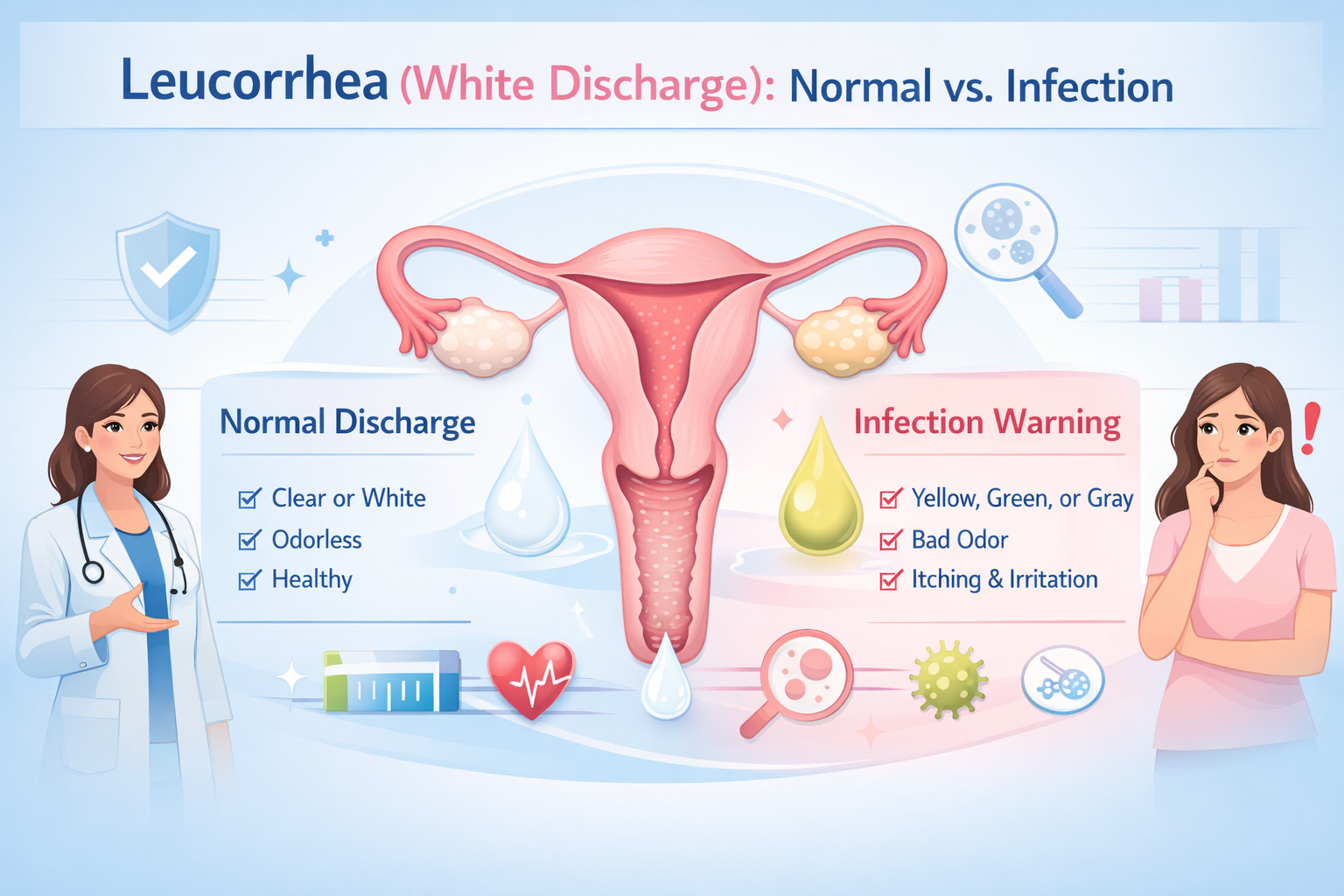
What Does Normal Discharge Look Like?
Normal discharge has a very specific profile:
- Color: Clear, milky white, or slightly off-white
- Texture: Thin to slightly sticky or gooey; may become more fluid around ovulation
- Smell: Mild or odorless - not sharp, pungent, or "fishy"
- Amount: Varies from person to person and throughout the menstrual cycle
- Sensation: No itching, burning, or discomfort
Every woman's baseline is slightly different. The goal is to know your own normal so that any departure from it becomes easier to recognize.
What Your Discharge Color Is Telling You
Color is the single most useful indicator of whether discharge is healthy or problematic. Here is a practical breakdown:
When color is accompanied by a foul odor, itching, burning, or pelvic discomfort - that combination is your signal to seek medical evaluation rather than attempt to do it your own home management alone.
Normal Causes of White Discharge
Not all leucorrhea is linked to infection. In fact, most white discharge has a perfectly healthy explanation tied to hormonal fluctuations:
Ovulation Around the middle of your menstrual cycle, estrogen levels peak and the body produces more discharge. It becomes stretchy, slippery, and egg-white in texture - this is your body's way of supporting fertility. It's completely normal and typically lasts two to three days.
Pregnancy Increased levels of estrogen and progesterone during pregnancy stimulate higher discharge production. This is the body's protective mechanism - the extra fluid helps prevent bacteria and infections from traveling up into the uterus. If you're pregnant and notice more discharge than usual, this is generally expected and normal.
Hormonal Birth Control Pills, patches, and hormonal IUDs can all alter the amount and consistency of discharge. You may notice more or thicker discharge in the first few months after starting or changing contraception.
Menopause Transition In the lead-up to menopause, hormonal changes can cause shifts in vaginal discharge - sometimes less, sometimes different in texture. These are normal physiological changes.
Stress and Lifestyle Factors Physical stress, dietary changes, lack of sleep, and certain medications can all temporarily affect discharge. This doesn't necessarily indicate an infection.
When White Discharge Signals an Infection
This is where the do it yourself approach has important limits. Certain changes in discharge - especially when paired with other symptoms - strongly indicate an infection that requires medical diagnosis and treatment.
Yeast Infection
A yeast infection (candidiasis) is one of the most common causes of abnormal white discharge. It occurs when Candida fungi overgrow in the vaginal environment.
What the discharge looks like:
- Thick and chunky, resembling cottage cheese
- Usually white or off-white
- Typically odorless, but the surrounding area feels intensely itchy
Other symptoms:
- Vaginal swelling or redness
- Burning during urination
- Pain or discomfort during sex
Yeast infections are not sexually transmitted - they can develop due to antibiotic use (which kills protective bacteria), high sugar intake, tight synthetic clothing, or hormonal changes.
Bacterial Vaginosis
Bacterial vaginosis (BV) occurs when the natural bacterial balance inside the vagina is disrupted and harmful bacteria overgrow. It is the most common vaginal infection in women of reproductive age.
What the discharge looks like:
- White or gray in color
- Thin and watery in texture
- Has a strong, unmistakable fishy odor - especially noticeable after sex
Other symptoms:
- Mild itching or irritation
- Burning during urination
- The odor is the most defining feature
BV is not classified as an STI, but sexual activity can disrupt vaginal pH and trigger it. It requires antibiotic treatment - it will not resolve on its own with hygiene alone.
Sexually Transmitted Infections
Certain STIs directly change the appearance and character of vaginal discharge:
- Trichomoniasis: Produces greenish-yellow, frothy discharge with a foul smell and significant itching or burning
- Chlamydia and Gonorrhea: May cause cloudy, yellow, or green discharge; sometimes there are no symptoms at all, making regular STI screening important
- These infections cannot be self-diagnosed or self-treated - medical testing and prescription antibiotics or antiparasitics are required
Do It Yourself Ways to Assess Your Discharge at Home
Before visiting a doctor, there are several do it yourself observation steps that can help you understand what you're experiencing and communicate it clearly to a healthcare provider.
1. Check the Color Consistently Look at your underwear or toilet paper in natural light. Is the discharge the same color it's always been, or has something shifted recently? Yellow, green, or gray are clear signals to act on.
2. Assess the Texture Is it the same thin, slightly sticky consistency you're used to? Thick and chunky texture - especially with itching - suggests a yeast infection. Watery and thin with a strong smell points more toward bacterial vaginosis.
3. Notice the Smell Healthy discharge has a mild, slightly acidic smell. A fishy odor - particularly one that intensifies after sex - is a key marker of bacterial vaginosis. A foul or pungent smell generally signals infection.
4. Check for Associated Symptoms Ask yourself honestly: Is there itching? Burning when I urinate? Pelvic pressure or pain? Swelling around the vaginal area? These accompanying signs narrow down the likely cause significantly.
5. Track Changes Over Your Cycle Discharge naturally changes throughout the month - thinner and more fluid around ovulation, thicker before your period. Keeping a simple mental or written note of your discharge across the month helps you distinguish cyclical normal changes from infection-related ones.
Do It Yourself Tips to Manage and Prevent Abnormal Discharge
When your discharge is normal but you want to maintain vaginal health, or when symptoms are mild and you're managing discomfort while awaiting a doctor's appointment, these do it your own strategies are practical and safe:
Maintain Good Hygiene - But Don't Overdo It
- Wash the external genital area daily with warm water - no soap inside the vaginal opening
- Never douche. Douching disrupts the natural bacterial balance and can actually cause or worsen infections
- Change underwear daily and after exercise
Choose the Right Clothing
- Wear loose-fitting clothing and breathable cotton underwear
- Avoid tight synthetic fabrics that trap moisture, as a warm, moist environment promotes bacterial and yeast overgrowth
Stay Hydrated and Watch Your Diet
- Drink adequate water daily to support overall body health
- Reducing refined sugar intake may help reduce yeast overgrowth, as yeast feeds on sugar
Urinate After Sex
- This simple habit reduces the risk of bacterial transfer into the urethra and vaginal area
Use Panty Liners Wisely
- If you experience heavier discharge that is otherwise healthy, a daily panty liner can help with comfort. Change it regularly - do not use scented liners as they can irritate the vaginal area
Consider Probiotics
- Research suggests that probiotics - particularly Lactobacillus strains - can support healthy vaginal flora. You can get these through fermented foods like yogurt or through supplements. Talk to a healthcare provider before starting a supplement routine
Avoid Scented Products
- Scented soaps, body washes, and feminine hygiene sprays near the vaginal area can irritate the delicate pH balance and trigger infections
What Tests Are Used to Diagnose Abnormal Discharge?
If your discharge changes and you visit a doctor, they may use several diagnostic tests to identify the cause:
- Pelvic Exam: The doctor visually inspects the vaginal area for redness, inflammation, or other signs of infection
- pH Test: Normal vaginal pH is 4.0–4.5. A reading above 4.5 suggests bacterial infection, as BV and trichomoniasis raise vaginal pH
- Wet Mount Test (Vaginal Smear): A sample of discharge is examined under a microscope - bacterial cells point to vaginitis, while yeast cells suggest candidiasis
- Gram Stain: A staining technique used to identify bacterial infections and distinguish them from other conditions
- Vaginal Culture: A discharge sample is grown in a lab to identify specific bacteria, yeast, or parasites like trichomoniasis
- STI Screening: Blood tests or swabs to test for chlamydia, gonorrhea, or other sexually transmitted infections
These tests are quick, typically painless, and give the provider precise information needed to prescribe the right treatment. Early diagnosis always leads to faster recovery and fewer complications.
When to See a Doctor
While many instances of white discharge are completely normal, the following situations require prompt medical attention:
- Your discharge has changed color - especially to yellow, green, or gray
- There is a persistent fishy or foul odor that doesn't resolve with normal hygiene
- You notice significant itching, burning, or swelling around the vaginal area
- You have pelvic pain or pain during urination
- You are pregnant and notice a sudden increase or change in discharge
- Your discharge looks like cottage cheese and is accompanied by intense itching
- You have multiple or recurring infections - this warrants further investigation
Do not attempt to self-diagnose or self-treat with over-the-counter products if you are unsure of the cause. Using the wrong treatment (such as an antifungal for bacterial vaginosis) can make the infection worse or mask its true cause.
Conclusion & Key Takeaways
White vaginal discharge - leucorrhea - is one of the most normal things a woman's body does. It is not dirty, unhealthy, or shameful. It is your body's built-in housekeeping and protective system for the reproductive tract.
Here's what to remember:
- Leucorrhea is normal when it is clear, white, or off-white, has a mild odor, and doesn't cause discomfort
- Color, smell, and texture are the three most important signals to watch - changes in any of these are your early warning system
- Yeast infections, bacterial vaginosis, and STIs are the most common causes of abnormal white discharge
- Do it yourself home checks - observing color, texture, smell, and accompanying symptoms - help you assess what's happening and communicate it clearly to a doctor
- Douching is never the answer - it disrupts vaginal balance and can make infections worse
- Prevention is possible through good hygiene practices, cotton underwear, probiotics, staying hydrated, and urinating after sex
- Medical tests like wet mount, pH testing, Gram stain, and vaginal culture are fast and effective at identifying the exact cause
- See a doctor if color, smell, or texture changes - especially if itching, burning, or pelvic pain are present
Your vaginal health is a reflection of your overall health. Learning to read the signals your body sends - and knowing when to act on them - is one of the most empowering things you can do for yourself.